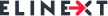Wearables for diabetes management are smart devices that continuously monitor glucose levels, activity, and health metrics. Powered by medical device software development services, they are designed for people with type 1 and type 2 diabetes, endocrinologists, and healthcare teams. Results include more accurate glucose control, fewer hypoglycemic episodes, and data-driven treatment decisions—improving quality of life and reducing long-term complications.
Diabetes wearables are transforming healthcare: according to MarketsandMarkets, the US market is expected to reach $12.94 billion by 2026. Continuous glucose monitoring devices reduce HbA1c levels by up to 0.40% and increase time spent in target range by 5.5%. A telemedicine app development company integrates this data into remote workflows, enabling preventative measures and reducing costly hospitalizations.
Over the last 100 years, the lifestyle of people has dramatically changed. In the past, people used to follow a more healthy diet: food was mostly organic, meals were much smaller and contained far fewer calories than today. Also, previously, people used to be physically active the biggest part of the day. In contrast, modern people eat too much, often fast food, and have a lack of physical activity throughout their days. All these contribute to a sedentary lifestyle and obesity, triggering the rise in the number of diabetes cases.
Diabetes management and monitoring require improved access to care delivery management solutions and diabetes wearables efforts in particular. Blood glucose level, blood pressure, heart rate, temperature, physical activity, diet, and some other factors should be considered. With the advent of diabetes wearables and custom HealthTech solutions, measuring and monitoring these factors becomes easier than ever.
In this blog post, we will take a look at some of the existing and coming wearables for diabetes that help or have the potential of helping diabetes patients monitor their medical parameters easily and enjoy a healthier life.
Diabetes Wearables for Patients
There is no doubt that connected devices will play a significant role in the future of healthcare. As to the management and monitoring procedures for patients with diabetes, the beneficial role of wearable devices is already apparent.
Today, people with diabetes can already use a range of connected devices that make their life a bit easier and a bit more relaxed. Such devices allow not just measuring physical activity, heart rate and temperature, but also continuously and effortlessly monitor their blood glucose level, body mass index, pulse wave velocity, sleep, activity, etc., as well as to detect inflammation and the risk of amputation. The variety of wearables for diabetes management is wide, and some of the most known forms existing today or coming in the nearest future are illustrated in the picture below.
What is Wearables Software for Healthcare?
Wearable software in healthcare is the application layer that collects, processes, and visualizes sensor data from wearable devices. For wearables for diabetes management, this means real-time CGM dashboards, insulin dosing algorithms, and electronic health record connectors. Professional wearable app development services ensure FDA/CE compliance, robust data security, and seamless integration with hospital and telemedicine platforms, transforming raw biometric data into actionable clinical insights.
Adopt wearables for diabetes today: real-time glucose information saves lives and reduces treatment costs.
Now let’s take a closer look at each of these devices.
Continuous Glucose Monitoring Systems Using Flash Drives
This concept includes wristbands, smartwatches, patches, smart shoes, and other wearable glucose monitoring devices. However, the most popular type of continuous glucose monitoring system using flash drives are devices that attach to the skin, typically on the abdomen or arm. These devices measure glucose levels every few minutes, giving users the ability to better manage their health.
Smart Contact Lenses
While contact lenses are typically used for vision correction, this is about to change. The development of new materials and the move toward minimizing electronics allow contact lenses to monitor the wearer’s health, such as blood sugar levels.
There is a partnership between Google and pharmaceutical manufacturer Novartis to develop contact lenses that will allow diabetic patients to track their blood sugar levels in real time using a mobile device.
Smart Wearable ECG Monitor
Another connected device that offers more convenient health monitoring for patients with diabetes, as well as for those with a family history of heart attacks or strokes, high blood pressure, high cholesterol, and excess weight, is a wearable ECG monitor. Existing devices, such as the Quardiocore, measure skin temperature, heart rate and heart rate variability, respiratory rate, and activity, analyzing these factors to provide users with valuable, potentially lifesaving information.
Smart Pill
This device is designed to free people with diabetes from the unpleasant task of multiple insulin injections per day. A pill the size of a small berry delivers insulin using a thin needle.
Smart Watches
Today, a wide range of smart watches are available, including those designed specifically for people who want to monitor their glucose levels. Using biosensors, these devices painlessly measure glucose levels throughout the day and night. The results are conveniently displayed on the watch screen.
Artificial Pancreas System
This system is designed to help people with type 1 diabetes maintain normal blood sugar levels by continuously monitoring blood glucose levels and using an algorithm to automatically deliver the right amount of insulin at the right time.
Smart Socks
Various types of smart socks have been developed, including for patients with diabetes, that measure insulin levels using biosensors, as well as temperature and inflammation. Most importantly, these wearables allow doctors to remotely monitor their patients and immediately notify them if any health parameters indicate a problem requiring medical intervention.
Smart Scales
Because diabetes-related complications are so serious, patients need to manage their weight to minimize the risk of cardiovascular disease and improve blood sugar levels. Smart scales provide information on BMI, visceral fat, water, as well as bone and muscle mass.
Key Benefits of Wearables for Diabetes
Wearables for diabetes offer five key benefits: continuous glucose monitoring, hypoglycemia prediction, improved time in target range, increased patient adherence, and remote monitoring capabilities. Together, these benefits enable both patients and physicians to proactively manage their condition, reducing the risk of complications and hospitalizations.
-
Access Real-Time Data and Trends Anytime
Diabetes wearables transmit glucose readings every 1–5 minutes to Healthcare professionals receiving population-level glycemic data without manual lab testing, reducing operational costs and enabling a proactive approach to treatment. PubMed, 2025 clinical studies show that continuous glucose monitoring increases time in target range by 5.57% in patients with diabetes.
-
Improved Adherence to Treatment Plans
Wearables for diabetes provide personalized reminders, medication reminders, and visual glucose feedback to help patients adhere to their daily treatment plans. Improved treatment adherence reduces the number of costly emergency visits and mitigates risks for payers, strengthening the economic case for digital diabetes management programs. According to PubMed, 2025 users of real-time continuous glucose monitoring systems demonstrate a 0.40% reduction in HbA1c levels in patients with type 2 diabetes compared to standard care, reflecting sustainable behavioral changes.
-
More Personalized Care Plans
Wearables for diabetes management generate detailed data on glucose patterns, activity, sleep, and dietary correlations that clinicians use to develop individualized treatment plans. Personalized protocols improve patient outcomes and differentiate digital healthcare offerings in a competitive market. According to PubMed, 2024 data-driven personalization leads to a 6.36% improvement in “Time in Target Range” in patients with type 2 diabetes when using therapy adjustments guided by continuous glucose monitoring systems.
-
Enhanced Potential for Remote Monitoring
Wearables for diabetes management devices transmit real-time health metrics to remote care teams, enabling virtual consultations and automated alerts without in-person visits. Remote monitoring expands patient reach, reduces overhead costs, and meets the growing demand for telemedicine services in chronic disease management. According to PubMed, 2023 CGM-based remote monitoring reduces the risk of all-cause hospitalization by 25% in patients with type 1 diabetes, providing clear clinical and economic value.
Diabetes management generates continuous streams of glucose, activity, and medication data that most clinical systems cannot process in real time, leaving critical patterns invisible to healthcare professionals. Elinext healthcare software development services bridge this gap by creating secure, interoperable CGM integrations and analytics dashboards. The result: faster clinical decisions, fewer adverse events, and measurable ROI for digital health providers.
Elinext Software Development Expert
Conclusion
Wearables for diabetes management are no longer optional as they have become the standard of modern glycemic care. The continuous glucose monitoring (CGM) market is expected to reach $15.81 billion in 2025, with HbA1c reductions of up to 0.40% and hospitalization risk reductions of 25%. Partnering with a EHR software development company ensures seamless integration of these devices with clinical records, transforming raw sensor data into coordinated, evidence-based patient care across the system.
Wearables for Diabetes: Terms Explained
-
Continuous Glucose Monitoring (CGM)
CGM is a wearable sensor system that automatically measures glucose levels in interstitial fluid every 1–5 minutes and displays the readings on a display. It replaces painful finger pricks by providing a continuous glucose curve that identifies trends, peaks, and troughs, enabling timely clinical and self-management decisions around the clock.
-
Interstitial Fluid Measurement
Interstitial fluid glucose measurement is a process in which CGM sensors measure glucose concentration in the fluid surrounding subcutaneous cells, rather than directly in the blood. A small electrochemical thread inserted under the skin oxidizes glucose molecules, generating a current proportional to the concentration, typically correlating with blood glucose levels with a physiological delay of 5–10 minutes.
-
Real-Time Glucose Streaming
Real-time glucose streaming is the continuous wireless transmission of CGM sensor readings to paired devices smartphones, smartwatches, or clinical platforms as data is generated. Using Bluetooth Low Energy, readings are received every 1–5 minutes, allowing patients and clinicians to monitor glucose trends in real time, instantly respond to alerts, and securely record data in cloud-based medical records.
-
Automated Insulin Delivery (AID)
Automated insulin delivery is a closed-loop therapy system that combines a CGM sensor, a control algorithm, and an insulin pump to automatically adjust the basal insulin dose based on real-time glucose readings. AID systems reduce the cognitive load of manual dosing, lower HbA1c levels, and significantly improve Time in Target Range especially at night, when the risk of hypoglycemia is highest.
-
Closed-Loop Control System
A closed-loop management system in diabetes management is a feedback mechanism in which the CGM sensor continuously feeds glucose data to a control algorithm, which automatically commands the insulin pump to deliver or suspend insulin. Often referred to as an “artificial pancreas,” this system mimics healthy pancreatic function, reducing manual intervention and improving glycemic stability throughout the circadian cycle.
-
Predictive Glucose Alerts
Predictive glucose alerts are proactive notifications generated by CGM software that predict a hypoglycemic or hyperglycemic event before it occurs, based on current glucose levels and their rate of change. Algorithms typically alert patients 15-30 minutes in advance, providing a critical window to reduce carbohydrate intake, adjust insulin doses, or contact a doctor preventing dangerous glycemic swings.
-
Time in Range (TIR)
Time in target range is the percentage of time a patient’s glucose level remains within the target range typically 70–180 mg/dL for most adults with diabetes. Measured by CGM, TIR is the new gold standard, complementing HbA1c, as it reflects day-to-day glycemic variability. A 5% increase in TIR is associated with a significant reduction in diabetes-related complications and improved quality of life.
-
Glucose Variability
Glucose variability refers to the degree of fluctuation in blood glucose levels over time, as measured by continuous glucose monitoring (CGM) metrics such as the coefficient of variation (CV) and standard deviation. High variability—frequent fluctuations between hypoglycemia and hyperglycemia—is independently associated with increased oxidative stress, cardiovascular risk, and complications, making its reduction a key therapeutic target alongside HbA1c.
-
Bluetooth Low Energy (BLE)
Bluetooth Low Energy is a wireless communication protocol designed for minimal power consumption, allowing CGM sensors and other wearable devices to continuously transmit data to paired devices without rapidly draining batteries. BLE operates in the 2.4 GHz band, supports a range of up to 10 meters, and is the standard connectivity level for most modern diabetes wearables, ensuring reliable, low-latency transmission of medical data.
-
Remote Patient Monitoring (RPM)
Remote patient monitoring is the use of connected devices, including continuous glucose monitoring sensors, blood pressure cuffs, and fitness trackers, to collect patient health data outside of traditional clinical settings and securely transmit it to healthcare teams.
FAQ
What are diabetes wearables?
Wearable devices for diabetes are sensor-based devices worn on the body to track glucose levels and health metrics. They are used to automate monitoring. Patients use them for daily management of both type 1 and type 2 diabetes without finger pricks.
How do wearables improve glucose monitoring?
Wearable devices improve glucose monitoring by providing continuous, automated readings every few minutes. They are used to identify trends. Doctors use them to adjust therapy before dangerous glucose spikes occur.
What is the biggest benefit of continuous glucose monitoring (CGM)?
The main benefit of CGM is that it eliminates gaps in monitoring. It is used to identify hidden patterns in glucose levels. Patients use it to reduce HbA1c by up to 0.40% and significantly increase the time spent in the target range.
How do wearables help prevent hypoglycemia and hyperglycemia?
Wearable devices prevent dangerous glucose-related events with predictive alerts sent 15-30 minutes before an event. They are used to take timely action. Patients use them to avoid emergency room visits and life-threatening episodes.
Do wearables support personalized diabetes care?
Wearable devices support personalized care by collecting data on individual glucose levels, activity, and sleep. They are used to create individualized treatment plans. Doctors use them to fine-tune insulin and dietary recommendations.
How do wearables enhance data-driven decision-making?
Wearable devices improve decision making by generating continuous streams of biometric data analyzed by AI algorithms. They are used to generate actionable insights. Healthcare teams use them for early intervention and optimized outcomes.