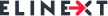Digital pregnancy support is transforming maternal and child health care through AI-powered analytics, wearables, and telemedicine. In 2025, the pregnancy digital health market was valued at $1.8 billion, with over 50% of pregnant women using digital pregnancy support apps. Medical device software development services enable the integration of wearables and remote monitoring, enabling early detection of complications and the provision of personalized care. AI-powered apps predict the risk of gestational diabetes, and IoT-based fetal monitors provide clinicians with real-time data. The future promises even wider adoption, interoperability, and personalized interventions, improving outcomes and reducing costs.
This is a real problem, since maternity health services are just as overworked and understaffed as in other niches, if not more. Every mother acts as a long-term patient, and to ensure her wellbeing throughout the course of pregnancy and childbirth one needs extensive human resources or advanced digital support.
The global pregnancy tracking app market size was valued at USD 301.32 million in 2024. It is projected to grow from USD 356.85 million in 2025 to USD 1380.97 million by 2033, registering a CAGR of 18.43% during the forecast period (2025–2033).
In this article, we’ll look at what the options for digital support in maternity are, how healthcare facilities can benefit from digitizing this field, and what has already been implemented.
What are the Digital Pregnancy Support Services?
Digital pregnancy support services include pregnancy digital health apps for symptom tracking, fetal movement monitoring, and mental health screening. Ovia Pregnancy and Baby Buddy offer educational content, appointment reminders, and community forums. Telemedicine platforms provide virtual consultations and 24/7 clinical support, while wearable devices monitor vital signs and fetal well-being. These services empower women, increase their self-efficacy, and improve their satisfaction during pregnancy.
What is the Role of Digital Services for Pregnancy Support?
Pregnancy digital health and mHealth app development services play a critical role in increasing access, engagement, and outcomes. They provide remote monitoring, early detection of complications, and personalized education. Digital platforms help manage gestational diabetes, track blood pressure, and provide psychological support. These services reduce unnecessary visits, lower costs, and ensure timely intervention, making pregnancy care more effective and patient-centered.
Use digital pregnancy support to provide safer, more thoughtful, and personalized care for mothers. Invest in innovative solutions to stay ahead of trends and improve outcomes for mothers and babies.
How Can the Maternity Niche Benefit from Digital Pregnancy Support?
For things to catch up, one has to introduce digital support into all areas of the pregnancy pathway: antenatal, labour, birth, and postnatal. Digital support should first and foremost include electronic medical records that are accessible at any time to both clinicians and patients.
In addition to electronic records, healthcare software companies propose tools that make it easier to manage and analyze large amounts of patients’ data. For example, an Elinext case study describes a Measure Management & Administration health analytics tool that’s integrated with Electronic Medical Records (EMR) software to help providers manage performance-based contracts and improve quality reporting measures.
Digital support can improve the safety of care, ensure better communication with health professionals, and take personalization of care to a whole new level. For example, women could complete personalised care and support plans online, which will not only free up midwife’s time but also ensure the mothers’ personal needs are being considered.
Initiatives and Examples of Digital Pregnancy Support
Pregnancy digital health apps such as Ovia and NHS MyCare provide symptom tracking, educational content, and direct communication with doctors. The PPSP program in the US has reduced preterm births and hospitalizations, while the NHS Midwifery Transformation Program has implemented interoperable medical records and digital tools, improving care coordination and patient satisfaction.
In the UK, the National Health Service created a long-term plan in which all paper notes should be replaced with digital services by 2023/2024. This digital maternity app was introduced as a pilot program that was available to 100 000 women in the UK. They can now access their test results, monitor their baby’s movements, keep a diary of their symptoms, and access their pregnancy notes.
Right now, there are four programmes that aim to digitize care for women in maternity services. Their goals are the following:
- ensure investment in electronic maternity records to reduce the administrative burden of information recording and sharing;
- provide women with quick and easy access to digital sources of information;
- create a digital tool that collects personal health records and returns personalised information;
- ensure these solutions are accessible to everyone involved outside the hospital settings.
What are Some Challenges for Introducing Digital Pregnancy Support?
Digital pregnancy support faces challenges such as inequalities in digital literacy, limited internet access, and privacy issues. Some women may find it difficult to use apps due to language barriers or lack of smartphones. Ensuring content quality, regulatory compliance, and equal access are crucial for successful implementation.
Introducing digital support into the maternity niche of healthcare obviously has its challenges. However, when it came to actual implementation, perceived challenges and real challenges faced by implementation teams differed a lot.
Even women who are socially disadvantaged report high levels of digital media usage. So as opposed to what was expected, there was no problem with adoption of new technology by pregnant people.
There were also concerns that staff would be reluctant to use new technology and a parallel paper system might emerge. This didn’t turn out to be the case.
Communication with health professionals and training of clinical staff was challenging, mainly due to inadequate human resources. The lack of opportunity for staff to ‘play’ on a training domain was also a major deficit. Hopefully, these challenges are being dealt with during current processes of digital support implementation.
The Four Digitization Programmes for Pregnancy Support:
-
Maternity Digital Maturity Assessment
Healthcare software development services support digital maturity assessments of maternity hospitals, such as the NHS DMA, which assesses digital capabilities and identifies gaps. 44 local maternity hospital systems in England use DMA reports to guide investments in digital infrastructure, ensuring readiness for expanded digital pregnancy support and improving the quality of care.
Digital pregnancy support helps obstetrics providers provide continuous care, early risk identification, and personalized guidance. Remote blood pressure and glucose monitoring enables timely intervention, reduces the risk of complications, and improves birth outcomes. Pregnancy digital health solutions also improve patient engagement and satisfaction.
-
Interoperable Maternity Records
Pregnancy digital health is currently focused on interoperable maternity hospital maps using standards such as SNOMED CT and FHIR. The NHS Maternity Records Standard ensures the seamless exchange of standardised records between healthcare settings, reducing duplication and promoting safer and more coordinated care.
-
Women’s Digital Care Record
Pregnancy digital health app, such as the Digital Pregnancy Tracker, provide women with direct access to their medical data, test results, and personalized recommendations. Over 100,000 women in the UK have accessed their digital tracks, increasing engagement and empowering them to actively participate in their own care.
-
A Digital Toolset
Digital pregnancy support includes comprehensive toolkits, including weekly recommendations, information on local services, and evidence-based resources. NHS.uk Maternity pages offer personalized content and service directories, helping women make informed decisions and receive support throughout their pregnancy.
Maternity apps often focus on providing informational, evidence-based content and emotional support. In terms of their actual features, they are often divided into three general categories:
- Tracking ovulation and fertility;
- Providing a digital mirror of pregnancy pathway;
- Providing access to nurses and specialists, navigating assisted reproductive technology, or managing care coordination.
“By 2025, pregnancy digital health and digital pregnancy support will revolutionize maternity care. By integrating AI, wearables, and secure digital platforms, we provide women and physicians with access to real-time information, personalized recommendations, and seamless communication, leading to improved outcomes and increased satisfaction with every pregnancy.”
Elinext Expert Quote
Conclusion
Digital pregnancy support and pregnancy digital health app are transforming the way healthcare is delivered. By 2025, more than 50% of pregnant women will use these solutions, and the market will reach $1.8 billion. Initiatives such as interoperable medical records, digital maturity assessment, and AI-based monitoring are improving outcomes, reducing costs, and increasing patient satisfaction. As software development services for medical devices evolve, digital pregnancy support will become even more personalized, accessible, and effective.
FAQ
What is digital pregnancy support?
Digital pregnancy support uses apps and platforms to educate, monitor, and communicate with expectant mothers. Apps track symptoms and offer real-time consultations, improving care and patient engagement.
Why is digital pregnancy support becoming popular?
It provides convenience, personalized care, and better outcomes. Over 50% of pregnant women use digital pregnancy support for easy access to information and remote monitoring.
What future trends are shaping digital pregnancy support?
Digital pregnancy support includes AI-powered analytics, integration with wearables, and compatible records. AI predicts complications, while wearables provide real-time monitoring and personalized interventions.
How does AI improve digital pregnancy support?
AI analyzes health data to predict risks and personalize care. AI-powered apps can detect the risk of gestational diabetes early, enabling timely intervention and improved outcomes.
How can wearable devices support pregnant women?
Digital pregnancy support wearables monitor heart rate, blood pressure, and fetal movements. IoT-enabled belts alert doctors to abnormalities, enhancing safety and peace of mind.
Are digital pregnancy apps safe to use?
Most digital pregnancy support apps are safe if they comply with privacy standards and regulatory requirements. Apps developed using medical device software services ensure data security and clinical validation.
Can digital pregnancy support help postnatal care?
Yes, digital pregnancy support extends to postpartum care, offering tools for mental health support, breastfeeding, and recovery tracking. Apps offer postpartum depression screening and virtual support groups.